Greggory Brandle, DO and Amy Tucker, MD
Western Reserve Hospital
DOI: http://doi.org/10.70709/4a9hut6ws9
Abstract
Case
In this case report, a middle-aged male on anticoagulation suffered a crush injury to the left arm and forearm that resulted in a compartment syndrome. The patient initially presented to the emergency room for x-rays that were negative. He was informed to come back the hospital if he developed signs or symptoms of compartment syndrome. Less than 12 hours later the patient returned with history and physical exam consistent with compartment syndrome.
Conclusion
Compartment syndrome, although not common, is a potential limb threatening condition. It is important to be able to recognize and properly treat due to its potentially devastating complications. A high index of clinical suspicion and understanding the risk factors is needed for timely diagnosis and treatment. Emergent fasciotomies need to be performed to minimize these complications.
Keywords – Compartment syndrome, fasciotomy, anticoagulation, fracture
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Abbreviations
Deep vein thrombosis (DVT), pulmonary embolism (PE), vacuum assisted closure (VAC), Post Anesthesia Care Unit (PACU), operating room (OR).
Case Report
Upper Extremity Compartment Syndrome in a 48-year-old male on Anticoagulation
Introduction
Compartment syndrome can occur when there is an increase in the pressure within a muscular compartment. Increased pressure decreases perfusion to the local area and distal extremity and can lead to irreversible muscle and neurovascular damage. Compartment syndrome can be caused by fractures, hemorrhage, crush injuries, reperfusion injuries, burns, or compression on a compartment. Seen more commonly in the lower extremity than in the upper extremity, compartment syndrome is diagnosed based on clinical exam. When there is high suspicion, an emergent fasciotomy is performed to limit irreversible damage. In this article a case of upper extremity compartment syndrome following a crush injury in a patient on therapeutic anticoagulation is presented.
Informed Consent
The information presented in this case report was gathered with the utmost care to protect patient confidentiality and identity. Patient consent was obtained for educational purposes with risks and benefits discussed.
Case Report
A 48-year-old male was seen in the emergency department in the afternoon after a large tractor tire fell on his left arm. He states he felt a pop in the arm and had immediate pain and swelling. He states he had difficulty moving his left arm after the injury but originally denied numbness or tingling distal to the injury. On exam compartments were soft. Range of motion was limited due to pain. Bruising was noted of the anteromedial arm and proximal forearm, but the patient was neurovascularly intact. Xray’s taken in the emergency department were negative for fractures or dislocations of the humerus, elbow, or forearm. The patient had a recent history of several lower extremity deep vein thromboses (DVT), as well as a subsequent pulmonary embolus (PE). He was switched from Eliquis to therapeutic Lovenox due to continued thrombosis. He was being worked up by hematology for causes of the multiple blood clots.
The patient was discharged home with pain medications and a sling with concern for distal biceps rupture versus ligamentous injury to his elbow. He was provided with proper education on reasons to return to the emergency department including signs and symptoms of compartment syndrome.
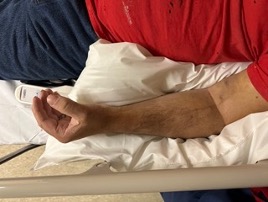
The patient returned to the emergency department 12 hours later with worsening pain of his left arm, numbness, tingling, and continued difficulty with range of motion. He stated that he took two Percocet tablets at home without any relief. On re-examination, the bruising had progressed. The patient presented with weakness of distal motor testing on the left compared to the right, diminished sensation of the left hand compared to the right, pain with passive flexion and extension of the wrist and elbow, and firmness of his forearm compartments and anterior arm. The posterior compartment of the arm was soft. Clinical appearance of the left upper extremity is seen in Figure 1.
Due to a high clinical suspicion for compartment syndrome in this patient, he was taken emergently to the operating room for fasciotomies of his forearm, anterior arm, and possible posterior arm with application of continuous negative pressure wound VAC.
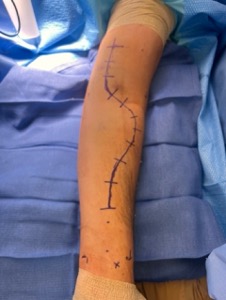
The patient was taken to the operating room. He was placed in the supine position with his arm on a hand table. Our planned incision (Figure 2.) was a curved S-shaped incision on the volar aspect of the forearm, starting over the flexor carpi radialis tendon distally, curving proximally over the mobile wad, then crossing the cubital fossa extending proximally towards the medial proximal arm. We started by exposing the radial artery distally and tracked it proximally. The fascia of the deep flexors was released. As we continued proximally the median nerve was identified and protected. Fasciotomy of the proximal forearm was completed. We then crossed the cubital fossa, released the lacertus fibrosis, and released the distal fascia of the anterior arm over the biceps and brachialis. The biceps tendon was noted to be intact. The final fasciotomy exposure and release can be seen in Figure 3. All three compartments of the anterior forearm were released. Hematoma was evacuated during the dissection and active bleeding was controlled with electrocautery. The wound was then irrigated, closed with a vessel loop shoelace technique, and a wound VAC was placed.
Post operatively in the Post Anesthesia Care Unit (PACU), the patient reported improved range of motion, improved pain, and improved sensation of his distal left upper extremity. On post operative day one, pain was improved, sensation returned to baseline when compared to the left, motor function distally was 5/5 except hand intrinsics, which was 4/5 when compared to the right.
The patient was returned to the operating room on post operative day 2 for repeat irrigation and debridement with primary closure. All muscle was noted to be viable with no active bleeding. On post-operative day 3, the patient was neurovascularly intact to baseline and was discharged home.

Discussion
Compartment syndrome is an orthopedic surgical emergency because it can be a limb-threatening condition. It can be caused by a multitude of injuries, most often associated with a fracture or soft tissue injury. Previous literature suggests that about 75% of all compartment syndrome are associated with a fracture. The remaining soft tissue problems include burns, vascular injuries, crush injuries, reperfusion injuries, improperly placed splints or casts, intense activity, malposition of a patient, and infection.(1-3) McQueen et al. looked at risk factors for compartment syndrome and found that 69% of compartment syndromes in their study had an associated fracture, half of the fractures being tibial shaft. Most of the patients were men under the age of 35. The second most common cause when a fracture was not present was a patient on anticoagulation or a patient with a bleeding disorder. (4)
When there is an elevation in pressure within a compartment, the pressure can exceed the venous capillary pressure. When the compartment pressure is higher than the venous pressure, the hydrostatic pressures in the compartment increase, and the arterioles become compressed. The perfusion to the surrounding and distal tissues decreases. When there is inadequate perfusion oxygenation decreases, the tissues do not get the nutrients they need, soft tissue ischemia begins and can lead to death of the tissues. (5-6)
The diagnosis of compartment syndrome is most often a clinical diagnosis based on the exam of the patient. The 5 “P’s” are very commonly described for what to look for on the clinical exam of a patient with suspected compartment syndrome. (7) Pain, pallor, paralysis, paresthesia’s, and pulselessness. Pain refers to pain out of proportion to what would be expected and pain with passive stretch of the muscles within the compartment. Pulselessness is more of a late finding and can mean that there is already irreversible damage. (1-3,5) When there is suspected compartment syndrome in an obtunded patient, there are instruments that can be used to obtain objective values to measure intracompartmental pressure. The most commonly used instrument today is the Stryker compartment pressure needle. A delta pressure less than 30 is suggestive of compartment syndrome. (8)
The goal of a fasciotomy is to decrease the pressure on neurovascular structures within the compartment. (5,6) Fasciotomy of the arm can be completed through one incision medially over the medial intramuscular septum. This allows for decompression of the both the anterior and posterior compartments on either side of the medial intramuscular septum. (5,9) The lazy S shaped incision allows for decompression of all forearm compartments (5,9-10) and can be extended proximally to the medial arm if needed for release of the arm compartments and can be extended distally to decompress the carpal tunnel. (9,10)
Management of the wound after fasciotomy can be challenging due to varying viability of the tissue and the edema present within the compartments. Primary closure initially is not often recommended. Many patients require return to the OR 48-72 hours following the index procedure for further debridement of viable tissues and to re-evaluate for further trauma and swelling. (3,5,11) The vessel shoelace technique is a way to gradually approximate the skin edges of the fasciotomy incision and allow for compartment edema to resolve. The technique involves running a vessel loop through skin staples at the edge of the incision in a shoelace looking fashion. The vessel loop is tightened each day until primary closure can be achieved. (11) A study was completed comparing patients with acute compartment syndrome who were closed using the vessel loop technique versus patients who were closed without the technique. They had a total of 25 patients, 13 of which were closed with the vessel loop technique and 12 without. The 13 patients in the vessel loop group did not require a skin graft whereas 6/12 patients who were closed without the vessel loop technique required a skin graft. (12)
Upper extremity compartment syndrome is a rare condition than can be encountered when there is an acute trauma to the upper extremity. The most common cause is an upper extremity fracture or crush injury. It is important to have a higher index of suspicion in a patient who is on anti-coagulation therapy or has a blood clotting disorder. Timely management and proper post operative wound management is important to minimize irreversible damage to the distal extremity.
References
- Tiwari A, Haq AI, Myint F, Hamilton G. Acute compartment syndromes. Br J Surg. 2002;89(4):397-412. doi:10.1046/j.0007-1323.2002.02063.x
- Maeckelbergh L, Colen S, Anné L. Upper arm compartment syndrome: a case report and review of the literature. Orthop Surg. 2013;5(3):229-232. doi:10.1111/os.12054
- Raza H, Mahapatra A. Acute compartment sy Raza H, Mahapatra A. Acute compartment syndrome in orthopedics: causes, diagnosis, and management. Adv Orthop. 2015;2015:543412. doi:10.1155/2015/543412
- McQueen MM, Gaston P, Court-Brown CM. Acute compartment syndrome. Who is at risk?. J Bone Joint Surg Br. 2000;82(2):200-203.
- Hanandeh A, Mani VR, Bauer P, Ramcharan A, Donaldson B. Identification and Surgical Management of Upper Arm and Forearm Compartment Syndrome. Cureus. 2019;11(10):e5862. Published 2019 Oct 8. doi:10.7759/cureus.5862
- Leversedge FJ, Moore TJ, Peterson BC, Seiler JG 3rd. Compartment syndrome of the upper extremity. J Hand Surg Am. 2011;36(3):544-560. doi:10.1016/j.jhsa.2010.12.008
- Garner AJ, Handa A. Screening tools in the diagnosis of acute compartment syndrome. Angiology. 2010;61(5):475-481. doi:10.1177/0003319710365145
- McQueen MM, Court-Brown CM. Compartment monitoring in tibial fractures. The pressure threshold for decompression. J Bone Joint Surg Br. 1996;78(1):99-104.
- Gelberman RH, Zakaib GS, Mubarak SJ, Hargens AR, Akeson WH. Decompression of forearm compartment syndromes. Clin Orthop Relat Res. 1978;(134):225-229.
- Matsen FA 3rd, Winquist RA, Krugmire RB Jr. Diagnosis and management of compartmental syndromes. J Bone Joint Surg Am. 1980;62(2):286-291.
- Asgari MM, Spinelli HM. The vessel loop shoelace technique for closure of fasciotomy wounds. Ann Plast Surg. 2000;44(2):225-229. doi:10.1097/00000637-200044020-00017
- Onoe A, Muroya T, Nakamura Y, et al. Efficacy of the shoelace technique for extremity fasciotomy wounds due to compartment syndrome. BMC Musculoskelet Disord. 2023;24(1):704. Published 2023 Sep 4. doi:10.1186/s12891-023-06849-1


